Restless Nights and Troubled Gums: The Connection Between Sleep Apnea and Periodontal Disease
What if your restless nights were silently damaging more than just your energy levels? Sleep is a fundamental component of human health, and disturbances in its quality or duration can have immense physiological consequences on one’s bodily systems. Today, recent research studies have been conducted in the hope of clarifying the relationship between sleep disorders, particularly obstructive sleep apnea (OSA), and oral health conditions such as periodontal disease; however, the underlying mechanisms of this relationship remain poorly understood. OSA, characterized by repeated upper airway obstruction during sleep, contributes to systemic inflammation, and it is known to trigger oxidative stress, both of which are also present in periodontal tissue breakdown. At the same time, periodontal disease, a chronic inflammatory condition affecting the underlying bone structure that supports the teeth, may not only be a result of poor oral hygiene but also a reflection of deeper physiological imbalances caused by disoriented sleep patterns. This paper will examine the intricate relationship between sleep disturbances, such as sleep apnea, and the development of periodontal disease through three case studies and two literature reviews. I argue that with increasing age, there is an increase in both the severity of sleep apnea and the progression of this gum-deteriorating disease.
As individuals experience the horrors of OSA, they often focus on the immediate symptoms of poor sleep, yet the chronic effects of this disorder can unknowingly deteriorate their oral health. In a study conducted by Pallavi et al. (2024), it was discovered that adult patients who exhibited severe obstructive sleep apnea had a greater risk of contracting periodontal disease as well. Specifically, these researchers found that those with severe OSA had a 78.4% chance of developing periodontal disease, while those with mild OSA had a significantly smaller chance (20.3%) of also exhibiting this disorder. Moreover, what was particularly interesting about this study was that the research methods utilized by the authors—a cross-sectional study, polysomnography, and the Apnea-Hypopnea Index (AHI)—allowed them to explore the broader health implications of OSA. Through this methodology, it was found that severe OSA is also linked to disorders such as hypertension, coronary heart disease, diabetes mellitus, and obesity (Pallavi et al., 2024), all of which are commonly associated with various oral health issues.
Furthermore, the study indicated that the severity of OSA tended to increase with age, creating a brutal cycle of health complications within this older demographic. Another interesting finding from this cross-sectional study was that “mild OSA (Stage 1) was found to be the most prevalent among participants, accounting for 59.2% of cases” (Pallavi et al., 2024). Through this, it can be observed that those with mild OSA are often undiagnosed until the disorder reaches a severity level that affects various other bodily inflammatory systems, influencing the development of periodontal disease. Thus, this study underscores the need to reconsider OSA not merely as a respiratory condition but as a multi-system disorder with serious oral health implications, especially among older adults who are primarily affected by this issue.
Sleep is a crucial natural practice that individuals need to function on a day-to-day basis. However, as individuals become older, they tend to prioritize sleep less and less. This lack of adequate sleep often causes these adults to experience poor sleep quality and varied sleep duration due to their increasingly demanding lifestyles and longer working hours. While sleep apnea is commonly associated with distorted bodily functions and inflammatory responses, it is not the only sleep disturbance that can have such effects. Within the systematic review conducted by Schmidlin et al. (2020), the researchers explored the broader connection between various sleep disorders and periodontal disease. One of the most compelling findings of this review was that low sleep quality, short sleep duration, and even excessively sleeping for long periods of time are significant factors in the development and progression of periodontal disease. This indicated that the negative impact on one’s oral health, due to not receiving enough good quality sleep, is not limited to those suffering from obstructive sleep apnea, as it also extends to individuals experiencing other forms of sleep disturbances in a process they refer to as “a vicious circle in itself” (Schmidlin et al).
Additionally, by the end of this study, the researchers discovered a second link between OSA and periodontal disease in the form of reverse causation. In other words, they found that “systemic inflammation induced by periodontitis and characterized by elevated levels of inflammatory biomarkers, such as cytokines, could, in turn, adversely influence sleep health.” (Schmidlin et al.). Through this, it can be seen that the relationship between OSA and periodontal disease is not simply a one-way street where troubled sleep can lead to negative oral health outcomes. Instead, both of these health issues can impact one another simultaneously since they are both systemic inflammatory conditions that worsen with limited oxygen intake. Like the natural process of sleeping, an individual’s oral health is a key factor in determining their overall well-being and quality of life. The maintenance of good dental health depends on a multitude of variables, such as one’s diet, oral hygiene routines, and general lifestyle decisions.
However, the research conducted by Movahed et al. (2023) suggests that oral diseases, like periodontal disease, could also be linked to various sleep disorders like OSA, which can further develop into physical and mental health issues. Through the use of the Oral Health Questionnaire (OHQ), the researchers of this case study were able to analyze the results of 6,161 participants who answered questions regarding their overall dental pain, bone loss, and even the emotional trouble suffered due to their oral health issues (Movahed et al., 2023). In this way, the study was able to conclude that those with a sleep disorder felt more embarrassed about their oral health in a way that worsened their mental health, broadening the scope of this often overlooked connection. Moreover, to develop a connection between sleep disorders and periodontal disease, the researchers also included questions about participants’ sleep trouble and morning drowsiness. Through this, Movahed et al. (2023) discovered that individuals experiencing sleep disorders exhibited a higher likelihood of poor oral health outcomes compared to those lacking a sleep disorder.
To support this notion, the researchers highlighted that there was a strong association between “obstructive sleep apnea in children and deteriorated oral health” as well as a “significant relation between sleep duration in individuals under the age of 60 and their oral health status” (Movahed et al., 2023). Through this, it can be seen that sleep is a critical factor in assessing the quality of one’s oral health from childhood to late adulthood. Evidence from this study also points to a reduced masticatory function in individuals with sleep disorders, such as OSA and snoring, due to their loss of teeth with age, which could potentially exacerbate periodontal disease and negatively affect one’s overall health. Lastly, as shown in the table below, Movahed et al. discovered that this relationship between OSA and periodontal disease also affects the vulnerable youth of today. It is clear that the connection between these two conditions is not limited to one specific demographic, but rather it is a widespread health concern.
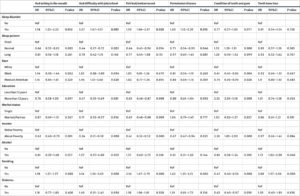
Figure 1: Multivariate analysis of sleep disturbances and covariate indicators by preventative measures linked to oral health outcomes
An inadequate duration of sleep can play a key role in the progression of periodontitis. In a study conducted by Wiener (2016), which examined a nationally representative sample from the 2009-2012 National Health and Nutrition Examination Surveys (NHANES), it was found that individuals who reported that their sleep was consistently poor had a much higher risk of developing periodontal disease than those who experienced adequate rest. Specifically, Wiener focused his research on adults over the age of thirty who had provided both oral health and sleep data in the questionnaire. From this, he was able to identify a clear positive association between inadequate sleep, which he defined as fewer than seven hours per night, and the presence of periodontal disease.
On the contrary, Wiener also noted that the relationship between these two conditions did not exist in sole isolation. For instance, he stated that “Other significant relationships with periodontitis were with diabetes; older age; male sex; being non-Hispanic Black, Mexican American, or other (as compared with being non-Hispanic White); lacking insurance coverage; being a current or former smoker (as compared with being a never smoker); having a lower federal poverty level, and having an education of high school graduation or less as compared with some college, technical school, or more.” This wide-ranging list of correlated factors proves that the risk of developing periodontal disease is deeply intertwined with broader socioeconomic, demographic, and systemic health disparities.
While Wiener’s research specifically centers on the connection between one’s sleeping patterns and oral health, these relevant variables suggest that sleep disturbances like OSA may serve as just one part of a more complex health puzzle. A study conducted by Hikmet et al. (2017) further discusses the influence of OSA on the development and progression of periodontal disease in a way that complements Wiener’s conclusions while providing a more targeted insight into their connection. For instance, Hikmet et al. stated that “the prevalence of severe periodontitis was significantly higher in the OSA group than the controls (48.2%),” thus supporting the idea that OSA contributes to more severe cases of periodontal disease. Additionally, similar to Wiener addressing multiple variables that could hinder the results of his study, Hikmet et al. discussed how factors associated with OSA, such as mouth breathing caused by oral dryness, raised the risk of exhibiting periodontal disease. Overall, it can be seen that the relationship between sleep disorders and one’s oral health is a multifaceted web that affects numerous other health issues and thus requires a need for a multifaceted approach when studying the connection between these two conditions.
In conclusion, obstructive sleep apnea and periodontal disease are deeply intertwined with one another in what one might call a “push-and-pull” relationship, fueled by systemic inflammation, oxidative stress, and disrupted oral health. From Pallavi to Schmidlin, Movahed, Wiener and Hikmet, the research from both case studies and literature reviews paints a clear picture that restless sleep truly does influence the development of troubled gums. Lastly, all of these studies emphasized the fact that as individuals age, the severity of both conditions does as well, revealing a hidden cycle that deteriorates both the quality of one’s sleep and oral health from childhood to late adulthood.
References
Gamsiz-Isik, H., Kiyan, E., Bingol, Z., Baser, U., Ademoglu, E. and Yalcin, F. (2017). Does obstructive sleep apnea increase the risk for periodontal disease? A case-control study. Journal of Periodontology, 88: 443-449. https://doi.org/10.1902/jop.2016.160365
Movahed, E., Moradi, S., Mortezagholi, B., Shafiee, A., Moltazemi, H., Hajishah, H., Shiahvoshi, S., Monfared, A. B., Amini, M. J., Safari, F., & Bakhtiyari, M. (2023). Investigating oral health among US adults with sleep disorders: A cross-sectional study. BMC Oral Health, 23(1), 996. https://doi.org/10.1186/s12903-023-03686-5
Pallavi, K., Amaranath, J., Das, N., Mukherjee, K., Das, A., & Katiyar, P. (2024). Determination of the association between obstructive sleep apnea and chronic periodontal disease: A cross-sectional study. Journal of Pharmacy and Bioallied Sciences. LWW. 16(Suppl 4), S3367–S3369. https://doi.org/10.4103/jpbs.jpbs_844_24
Schmidlin, P., Khademi, A., & Fakheran, O. (2020). Association between periodontal disease and non-apnea sleep disorder: A systematic review. Clinical Oral Investigations, 24(10),3335-3345. https://doi.org/10.1007/s00784-020-03475-2
Wiener, R. C. (2016). Relationship of routine inadequate sleep duration and periodontitis in a
nationally representative sample. Sleep Disorders, 2016, 1–6. https://doi.org/10.1155/2016/9158195
