Fats, the New Friends of the Celiacs

Introduction
In a world where bread symbolizes nourishment, this staple poses a life-threatening battleground in one of medicine’s most tragic paradoxes. Nearly 2 million people in the US alone suffer from Celiac disease, an autoimmune disease where the body’s immune system reacts adversely to gluten intake and destroys villi, which are microscopic finger-like projections in the small intestine that multiply its inner surface area, creating vastly more contact points for food particles and thereby enabling efficient nutrient absorption. Their destruction can lead to long-term nutrient deficiencies in Celiacs without a clear solution. This research paper examines the results from a 2015 study by Choi et al. from the National Library of Medicine, which showed that a high-fat diet improved villi growth in male mice with part of their small intestines surgically removed, and hypothesizes that a high-fat diet may help Celiacs regrow their villi, providing an active cure rather than simply abstaining from eating gluten and waiting for villi to naturally regrow.
Celiac Disease’s Impact on Villi and Nutrient Absorption
The surface-area-to-volume (SA:V) ratio shows that as objects get bigger, their volume increases faster than their surface area. Biologically, it is important for cells and tissues to maintain a high SA:V ratio to facilitate efficient movement of nutrients and wastes through the cell membranes. The same applies to villi, which are folds in the small intestine wall that multiply its surface area and maximize the nutrients absorbed as digestion progresses.
The research article “Generation of Intestinal Surface: an Absorbing Tale” examines the evolutionary processes that led to the development of villi and underscores the importance of villi for increasing the SA:V ratio of the small intestine (Walton et al.). Most importantly, this article mentions that villi are essential for proper nutrient absorption and that health conditions affecting villi may also cause nutrient deficiencies. In addition, the article “Celiac Disease – Symptoms and Causes” covers the general symptoms of Celiac disease and its role in villi destruction, which leads to long-term nutrient deficiencies (Mayo Clinic). There is also no definitive cure for this villi destruction, and Celiacs must wait for them to naturally regrow, an issue that could potentially be explored to aid villi regrowth.
The Research Plan
The main symptom of Celiac disease that this research seeks to address is villi damage, which will be explored by consolidating information from the research article “High-Fat Diet Enhances Villus Growth,” a research article that compares the use of a high-fat diet with a regular diet in rodents to increase villi growth (Choi et al.). The results from this experiment will serve as the main data used to test the hypothesis for this research, which is that a high-fat diet will promote villi growth and benefit health conditions involving villi destruction, such as Celiac disease. This can help prevent long-term nutrient deficiencies in Celiacs, which are known to be especially detrimental in children by causing slow physical and neurological development and sometimes a failure to thrive in infants (“Celiac Disease”). From a scholarly perspective, this research focuses on finding an original treatment to address the villi destruction resulting from Celiac disease. Such an objective is unique because there is no definitive cure for Celiac disease, and any damaged villi must normally regrow. The discovery of a potential villi growth promoter would significantly decrease the number of Celiacs suffering from long-term nutrient deficiencies and the consequences that would follow.
The Results
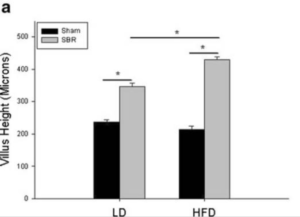
The research article “High-Fat Diet Enhances Villus Growth” by Choi et al. examines the difference in villi growth between two groups of male mice, some of which had undergone a small bowel resection, where part of the small intestine is surgically removed, and the remaining small intestine tract generally faces villi destruction, while others underwent a sham surgery with no lasting medical impact. The two groups were fed either a regular rodent diet or a high-fat diet, and using the combination of diet and whether or not the small bowel resection occurred, the researchers monitored villi growth. Figure 1A shows that in the mice that had a small bowel resection, a high-fat diet resulted in significantly higher villi growth compared to the regular rodent diet, while there was no discernible difference in mice that had the sham surgery.
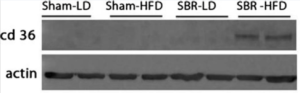
In addition, Figure 6 represents the results from a Western Blot procedure conducted to measure the amount of the CD36 protein, which transports fatty acids within cells, produced in the cells of these various mouse groups. The faint gray lines under the SBR-HFD category show that only the mice that both experienced villi destruction from the surgery and consumed a high-fat diet were able to produce the CD36 protein, which may have impacted the rates of villi growth. These results suggest that the high-fat diet helped boost villi growth in the mice that had small bowel resections, which was important since these mice were prone to short gut syndrome, where there has been a loss of villi that could hamper nutrient absorption, and villi regrowth is necessary to ensure normal function. This research also indicates that villi atrophy acts as a switch for the use of a high-fat diet to promote faster villi growth, which can be applied to Celiac disease since it also causes villi to be destroyed by the body’s severe immune responses.
While further investigation is still necessary, this experiment provides a starting point for using a high-fat diet to improve the rate of villi growth after any villi damage occurs. This data is consistent with the hypothesis generated, and it seems that a high-fat diet may promote villi growth and speed up the regeneration of villi when it has been destroyed.
Analysis
The data from the research paper by Choi et al. shows that it is worth exploring this hypothesis and extending these results to Celiac disease. Since this study does not deal with Celiac disease directly, this project instead examines the specific genes and proteins targeted in the experiment to consider applying the results to Celiac disease. Before the results from this experiment can be applied fully to Celiac disease, it is important to consider that the research paper only considered male mice that had undergone small bowel resections, and if these results were to be generalized to Celiac disease and other related conditions, further research must be conducted using a more diverse population of organisms and eventually humans. It is essential to research the potentially adverse impacts of high-fat diets on Celiacs. If a high-fat diet is suitable, it is also necessary to determine distinctions in what types of fat, such as plant-based or animal-based, and how much of these fats would produce the best results in villi growth, while also ensuring that the health of people with Celiac disease is not harmed. While there is no research specifically examining this relationship, this paper hypothesizes that natural and unsaturated fats would be best suited for Celiacs looking to promote villi growth using a high-fat diet. According to the article “The Best Gluten-Free Foods To Eat If You Have Celiac Disease” by Health, sources like olives, avocados, fatty fish such as salmon, nuts, and seeds are excellent sources of fat for Celiacs because they help the body absorb fat-soluble nutrients like Vitamin D while preventing side-effects of consuming fats, such as blocked arteries and heightened risk for cardiovascular disease. It is also essential to maintain balance while consuming these foods because fats are dense in calories, and overeating them can cause obesity and further health risks.
Conclusion
The results of this project show that a high-fat diet can increase the rate of villi growth compared to a regular diet in male mice that have had a small bowel resection. Given that this experiment started off with mice, the comparison of a high-fat diet versus a normal diet could be expanded to other animals and eventually humans, all while fulfilling ethical considerations and testing for any harmful side effects of a high-fat diet on Celiacs. This project is headed towards combining the phenomenon of a high-fat diet increasing villi growth in rodents with the situation of Celiac disease, where villi are also damaged due to extreme immune responses. This research aims to lead to an active treatment of the villi destruction in Celiac disease and prevent Celiacs from having to deal with the prolonged loss of villi, nutrient deficiencies, and the resulting side effects. These conclusions could potentially be applied to other conditions that also cause damaged villi and eventually contribute to the scientific field’s focus on applied science and finding solutions to health conditions that once had no definitive cure.
Works Cited
“The Best Gluten-Free Foods To Eat If You Have Celiac Disease.” Health, https://www.health.com/celiac-disease-diet-8709370. Accessed 18 Apr. 2025.
“Celiac Disease – Symptoms and Causes.” Mayo Clinic, https://www.mayoclinic.org/diseases-conditions/celiac-disease/symptoms-causes/syc-203 52220.
Choi, Pamela M., et al. “High-Fat Diet Enhances Villus Growth During the Adaptation Response
to Massive Proximal Small Bowel Resection.” Journal of Gastrointestinal Surgery: Official Journal of the Society for Surgery of the Alimentary Tract, vol. 18, no. 2, Feb. 2014, pp. 286–94. PubMed Central, https://doi.org/10.1007/s11605-013-2338-7.
Walton, Katherine D., et al. “Generation of Intestinal Surface: An Absorbing Tale.” Development (Cambridge, England), vol. 143, no. 13, July 2016, pp. 2261–72. PubMed Central, https://doi.org/10.1242/dev.135400.
