Is Poor Emotional Regulation Associated with Increased Risk-Taking Behavior in Children Diagnosed with ADHD vs. Typically Developing (TD) Children?

i. Abstract
This study investigates whether poor emotional regulation is associated with increased risk-taking behavior in children diagnosed with Attention-Deficit/Hyperactivity Disorder (ADHD) compared to typically developing (TD) peers. Utilizing data from 152 children ages 10- 13 years in the BrainMAP study, emotional regulation was assessed by the parent-report on the Emotion Regulation Checklist (ERC), and risk-taking behavior was measured using the Balloon Analogue Risk Task (BART). While children diagnosed with ADHD exhibited poorer emotional regulation than TD children, emotional regulation was not a significant predictor of risk-taking behavior in either group. Instead, age emerged as a more consistent predictor, with older children demonstrating higher levels of deliberate and impulsive risk-taking. These findings suggest that while poor emotional regulation is a prominent feature of ADHD, it may not directly contribute to risk-taking as measured by the BART. Future research should examine older adolescents to better understand how developmental changes in emotional regulation and decision-making influence real-world risk-taking over time.
ii. Introduction
Children diagnosed with Attention-Deficit/Hyperactivity Disorder (ADHD) are at heightened risk for engaging in a broad spectrum of risky behaviors, including substance use, unsafe sexual practices, and dangerous driving (Molina et al., 2018). Real-life risk-taking behavior (RTB) is defined as “engagement in behavior that is associated with some probability of undesirable results” (Bunford et al., 2015). While impulsivity has long been viewed as a core symptom driving such behavior, growing evidence suggests that poor emotional regulation (ER) may play a critical and underrecognized role (Bunford et al., 2015; Stralen, 2016).
ADHD & Risk Taking
ADHD is defined as a neurodevelopmental disorder, characterized by inattention, hyperactivity, and impulsivity, with a prevalence of around 5.3-7.2% in children and adolescents (Asadi et al., 2021; Shoham et al., 2016; Stralen, 2016). Beyond its diagnostic symptoms, ADHD
has been consistently associated with increased engagement in real-world risk-taking behaviors (Pollak et al., 2019). In a longitudinal study analyzing substance use through adolescence into early adulthood after childhood-diagnosed ADHD, Molina et al. (2018) found that more children with ADHD were early substance users and there was a slightly faster escalation of substance use in adolescence. For example, 33% of adults with childhood ADHD used marijuana weekly compared to 21% of the normative group (Molina et al., 2018). Furthermore, 36% of the adults with childhood ADHD vs. 18% of the normative group reported cigarette smoking (Molina et al., 2018). These findings suggested a possible mediational pathway that childhood ADHD led to early substance use, later heavy substance use, and eventually the possibility of substance use disorder in adulthood (Molina et al., 2018).
One widely studied mechanism underlying this association is altered reward sensitivity. A meta-analysis by Dekkers et al. (2016) suggested that individuals with ADHD may demonstrate a heightened focus on immediate rewards and, consequently, an ignorance of possible losses, resulting in suboptimal decision making. According to Pollak et al. (2016), suboptimal decision-making might result from differences in reinforcement learning, individuals’ perceptions of the risks and benefits associated with various choices, as well as a range of personal traits and contextual factors. Impaired reward processing is especially apparent in experimental tasks designed to measure risk-taking behavior, such as the Balloon Analogue Risk Task (BART) and the Iowa Gambling Task, in which children diagnosed with ADHD often persist in disadvantageous choices despite repeated negative feedback (Dekkers et al., 2016).
ADHD & Emotional Regulation
In addition to the well-known symptoms of impulsivity, hyperactivity, and inattention, poor emotional regulation has been increasingly recognized as a common difficulty among children with ADHD. Emotional regulation refers to an individual’s ability to modulate the speed, intensity, and deescalation of the physiological, experiential, and behavioral expression of emotion in a manner congruent with optimal functioning (Bunford et al., 2015). Many authors refer to poor emotional regulation as “emotional dysregulation,” defined as an inability to exercise these modulatory processes to a degree that results in functioning meaningfully below baseline (Bunford et al., 2015).
Children with ADHD often display heightened emotional reactivity, low frustration tolerance, and difficulty calming down once emotionally aroused (Bunford et al., 2015; Stralen, 2016). Although poor emotional regulation is not included in the diagnostic criteria for ADHD, a substantial number of children with the disorder experience emotional challenges that have been linked to increased social problems, poorer academic performance, and more severe behavioral issues (Bunford et al., 2015). Several studies indicate that these emotional challenges are intrinsic rather than secondary to comorbid disorders; for example, nearly 47% of children with ADHD displayed high levels of emotional lability compared to 15% of children without ADHD, which was strongly linked to increased aggression, depression, and overall impairment (Stralen, 2016).
The neuropsychological mechanisms underlying this association have been explored through models such as Barkley’s (1997) executive function theory, which suggests that poor behavioral inhibition undermines the development of self-regulation systems, including emotional regulation. Consistent with this model, children with ADHD exhibit greater emotional reactivity to positive and negative stimuli and perform worse on tasks requiring emotional control, particularly under stress (Stralen, 2016). Poor emotional regulation in ADHD is also associated with distinct physiological and neural signatures, including abnormal amygdala–anterior cingulate cortex connectivity and atypical autonomic nervous system activity, such as abnormal respiratory sinus arrhythmia (Stralen, 2016).
Importantly, not all children with ADHD demonstrate emotional difficulties to the same degree. Children with ADHD and poor emotion regulation exhibit significantly more behavioral problems, peer rejection, and functional impairment than those with intact emotional control, supporting the presence of meaningful subgroups within the ADHD population and highlighting the importance of evaluating emotional functioning alongside core symptoms (Bunford et al., 2015).
Interplay Between ADHD, Poor Emotional Regulation, and Risk-Taking Behavior
Although both ADHD and poor emotional regulation independently contribute to increased risk-taking behavior (RTB), growing evidence suggests that their co-occurrence may significantly amplify the risk of maladaptive behavior. Children and adolescents with ADHD who also struggle with managing emotional responses are more likely to engage in maladaptive risk-taking across a range of domains, including substance use, reckless driving, and unsafe sexual behavior. This may be due to the way emotional reactivity compounds with existing impulsivity and reward sensitivity, which leads to decisions that prioritize immediate emotional relief or stimulation over long-term consequences (Pollak et al., 2019; Bunford et al., 2015).
Poor emotional regulation may impair a child’s ability to pause, reflect, or tolerate frustration, which are capacities that are already compromised in ADHD due to deficits in executive functioning. As a result, emotionally charged situations may overwhelm cognitive control systems, increasing the likelihood of reactive, high-risk behavior. For example, emotionally dysregulated youth with ADHD may engage in impulsive substance use or confrontational behavior as a form of coping or emotional release (Bunford et al., 2015).
Recent findings complicate this picture. In a study by Asadi et al. (2021), both ADHD symptoms and poor ER were correlated with increased risk-taking behavior. However, when analyzed together, only ADHD symptoms, particularly inattention, were found to predict RTB (Asadi et al., 2021). This suggests that while poor emotional regulation contributes to the broader profile of ADHD, it may function as a moderating factor that can intensify risk in those already exhibiting ADHD-related traits. These results point to the importance of considering both cognitive and emotional pathways to risk. While impulsivity and reward-seeking explain some risky behavior, poor emotional regulation may alter how individuals respond under emotional stress or frustration, contexts in which risk-taking becomes more likely. This interaction may be especially relevant during adolescence, when both emotional intensity and the opportunity for risky behavior increase.
Taken together, the interaction between ADHD and poor emotional regulation highlights the need for a more nuanced understanding of risk behavior in this population. Targeting emotional regulation in intervention efforts may not only reduce emotional distress but also mitigate associated risk-taking behaviors. Despite growing recognition of these associations, it remains unclear whether poor emotional regulation has a distinct and measurable role in predicting risk-taking behavior, particularly when comparing children with ADHD to typically developing children. Clarifying this relation is essential for identifying which children are most vulnerable and for developing targeted interventions that address both cognitive control and emotional regulation processes. The current study addresses this gap by investigating whether poor emotional regulation is associated with increased risk-taking behavior in children, and whether the association differs between children diagnosed with ADHD and their typically developing peers. We hypothesize that: (1) Children with poor emotional regulation will engage in higher levels of risk-taking behavior; (2) Children diagnosed with ADHD will demonstrate worse scores on emotional regulation measures compared to typically developing children.
iii. Methods
Participants
Participants were 152 children ( n = 93 males, n = 59 females) (Appendix B) between the ages of 121 and 159 months (approximately 10-13 years old; M = 136.5 months) (Appendix C) who completed Wave 1 of the BrainMAP study. The sample included two diagnostic groups: 102 children diagnosed with ADHD and 50 typically developing (TD) children. Diagnostic classification was determined based on existing BrainMAP records. Participants were included if they completed both the parent-report Emotion Regulation Checklist and the Balloon Analogue Risk Task (BART) and did not withdraw from the study later. Children with missing data on the key measures were excluded from analyses.
iv. Measures
Emotion Regulation Checklist (ERC) – Parent Version
Emotional functioning was assessed using the parent-report version of the Emotion Regulation Checklist (ERC), a 24-item questionnaire designed to capture children’s typical emotional expression and regulation. Items are rated on a 4-point Likert scale (1 = rarely/never, 4 = Almost always). The ERC yields to subscales: Emotion Regulation (adaptive skills) and Lability/Negativity (emotional instability). For example, an item from the Emotion Regulation subscale asks, “Can say when she/he is feeling sad, angry, or mad”. In contrast, an item from the Lability/Negativity subscale asks, “is easily frustrated.” Higher scores on the Emotion Regulation subscale indicate greater regulator capacity. In comparison, higher scores on the Lability/Negativity Subscale reflect greater emotional reactivity. The primary analyses were run using the Total Emotion Score, and subscale scores were used in secondary analyses.
Balloon Analogue Risk Task (BART)
Risk-taking behavior was assessed using a computerized version of the Balloon Analogue Risk Task (BART). In this behavioral task, children press a button to inflate a virtual balloon, earning points with each pump. However, each additional pump increases the probability of the balloon bursting, which would result in no points for that trial. Participants may stop inflating at any time and bank the points. The primary outcome variable used was the adjusted number of pumps, defined as the average number of pumps on trials where the balloon did not explode. This measure reflects deliberate risk-taking, with higher scores indicating a greater willingness to take risks in pursuit of potential rewards. On the BART, participants with ADHD inflated the balloon more times, finding a medium effect size, suggesting greater risk-taking compared to typically developing controls.
However, some studies have found no increase in risk-taking when reward probabilities are equalized, indicating that ADHD-related risk behavior may reflect impulsive suboptimal decision-making rather than a true preference for risk (Pollak et al., 2016). Secondary outcomes included the number of balloon explosions and total points earned. The number of explosions represents the total number of balloons that burst during the task. A higher number of explosions may suggest poor risk estimation or a tendency to engage in risk without regard for potential loss. Total reward was measured as the total points earned across trials and reflects successful risk-taking attempts. Lower total rewards may indicate overly cautious behavior (cashing out too early) or excessive risk-taking that leads to balloon explosions and forfeited earnings.
Design and Statistical Analysis
The study used a between-subjects design, comparing children diagnosed with ADHD to typically developing peers. The primary analysis employed linear regression to investigate whether poor emotional regulation predicted risk-taking behavior, operationalized as the adjusted number of pumps on the BART. Predictor variables included emotion regulation scores, age (continuous), sex (categorical), and diagnostic group (ADHD vs. TD). Subgroup analyses were conducted separately for the ADHD and TD groups to test whether the association between emotional regulation and risk-taking differed by diagnostic status. Secondary regression analyses were conducted using the number of explosions as the outcome variable. Balloon explosions
were selected as a secondary outcome to assess a distinct form of risk-taking behavior. All analyses were conducted using R-Studio statistical software, with thresholds set at p < .05.
v. Results
Group Differences in Risk-Taking
Visual comparison of risk-taking behavior by diagnostic group revealed that TD children exhibited slightly higher average adjusted number of pumps compared to children diagnosed with ADHD (Figure 1). However, this difference was not statistically significant, and variability in performance was similar across groups.
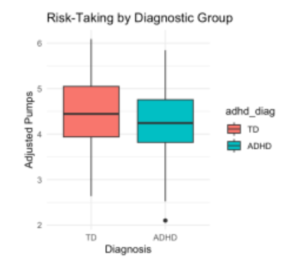
Figure 1: Risk Taking by Diagnostic Group
Full Sample Regression
A linear regression was conducted to examine whether the total emotion regulation score predicted risk-taking behavior on the BART. The model included total ERC score, age, sex, and diagnosis group as predictors of risk-taking, measured by adjusted number of pumps. The overall model was statistically significant (F(4, 147) = 2.50, p = .045), explaining 6.4% of the variance in adjusted pumps (R² = 0.064). However, the total ERC score was not a significant individual predictor of risk taking (p = .164); instead, age (p = 0.185) and diagnosis group (p = .0265) were the only significant predictors in this model (Figure 2).

Figure 2: Scatterplot of Total Emotion Regulation Score vs. Adjusted Pumps (Full Sample)
A follow-up regression tested the Emotion Regulation subscale as a predictor of adjusted number of pumps. This model approached significance but was not statistically significant (F (4, 147) = 2.07, p = .087), explaining 5.3% of the variance (R² = .053). Thus, emotion regulation itself was not a significant predictor of risk-taking at the individual level (Figure 3).
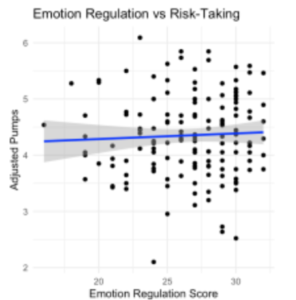
Figure 3: Scatterplot of Emotion regulation vs. Adjusted Pumps for the (Full Sample)
Subgroup Analyses by Diagnostic Group
To further explore whether the diagnostic group moderated the relationship between emotional functioning and risk-taking, separate regression models were conducted for the ADHD and TD subgroups using the ERC score, age, and sex as predictors of adjusted pumps (Figure 4). In the ADHD group, the model was not statistically significant (F(3, 98) = 1.28, p = .29, R² = 0.038). Total ERC was not a significant predictor (p = .303). In the TD group, the model was also not significant (F (3, 46) = 1.26, p = .30, R² = 0.076). Total ERC was again not significant (p = .176), although age approached significance in both groups (p = .07). See Appendix D for a table of significant values.
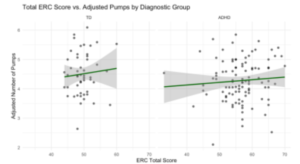
Figure 4: Side-by-Side Scatterplots of total ERC vs. Adjusted Pumps by Diagnostic Group
Age as a Predictor of Risk-Taking
Given the consistent trend of age approaching or reaching significance in prior models, a secondary analysis was conducted using age as the only predictor of risk-taking. Age significantly predicted the adjusted number of pumps in the full sample (p = .018), suggesting that older children tended to take more calculated risks on the BART (Figure 5).
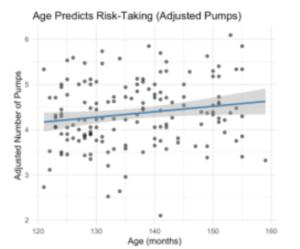
Figure 5: Scatterplot of the Relationship Between Age and Adjusted Pumps
A separate model was also conducted with the number of balloon explosions as the outcome, capturing a more impulsive or poorly regulated form of risk-taking (Figure 6). In this model, age was again a significant predictor (p = .003), indicating that older children were more likely to push the limits of the task and experience explosions.

Figure 6: Scatterplot of the Relationship Between Age and Number of Explosions
vi. Discussion
The current study examined whether poor emotional regulation is associated with increased risk-taking behavior in children and whether this relationship differs between children diagnosed with ADHD and their typically developing peers. We hypothesized that (1) children with poorer emotional regulation would exhibit higher levels of risk-taking on the BART and (2) children diagnosed with ADHD would demonstrate significantly poorer emotional regulation than TD children.
While the full sample regression model predicting risk-taking was statistically significant, emotional regulation was not a significant individual predictor of risk-taking on the BART. Similarly, subgroup analyses revealed that there was no significant relationship between emotional regulation and risk-taking within either the ADHD or typically developing groups. These findings do not support the first hypothesis. However, consistent with the second hypothesis, children diagnosed with ADHD did exhibit poorer emotional regulation scores compared to TD children.
Interestingly, age emerged as a consistent predictor of risk-taking behavior across models. Older children showed higher adjusted pump counts and experienced more balloon explosions. This suggests a developmental increase in risk engagement and possibly reflects improved task understanding or a greater willingness to test limits. This finding aligns with developmental neuroscience research, which suggests that adolescence is characterized by increased reward seeking and a shift in risk tolerance.
Given prior literature suggesting that emotional reactivity amplifies impulsive decision making in ADHD, the lack of a direct relationship between emotional regulation and risk-taking behavior was somewhat unexpected (Pollak et al., 2019; Asadi et al., 2021). One possible explanation is that the BART primarily measures reward sensitivity and calculated risk, rather than emotion-driven or reactive decision-making. Poor emotional regulation may be more strongly related to real-world risk-taking that involves social-emotional triggers, such as peer
influence, stress, or anger. For example, Asadi et al. (2021) found that ADHD symptoms, particularly inattention, predicted RTB even when controlling for emotion regulation, suggesting that ER may act as a moderator or amplifier, rather than a direct driver of risky behavior.
vii. Conclusion
Overall, the findings highlight that while poor emotional regulation is a key characteristic of ADHD, it may not directly predict task-based risk-taking in middle childhood. Instead, age related developmental changes appear to play a more prominent role in shaping risk behavior. These results underscore the need to explore how emotional and cognitive factors evolve, particularly in older adolescents, to better understand the real-world implications of ADHD and challenges with emotional regulation.
Limitations
Several limitations should be considered. First, the emotion regulation measure was based on the parent-report and may not fully reflect the child’s internal regulation capabilities. Data from multiple informants or observational data might yield different results. Second, the BART, while widely used, captures a narrow form of risk-taking that may not generalize to real world contexts involving emotional or social stakes. Third, the cross-sectional design limits our ability to infer causality or examine how emotional regulation influences RTB development over time.
Future Directions
Future research should consider longitudinal designs and a broader range of risk-taking tasks, particularly those involving emotionally or socially salient decisions. Given the developmental nature of both emotional regulation and risk-taking, future work could explore
these questions using Wave 3 data from the same BrainMAP participants. By comparing emotion regulation scores and BART performance across waves, researchers can examine how developmental changes in emotional functioning relate to real-time risk-taking behavior. This approach may help clarify whether age contributes to more controlled, deliberate risk-taking or if increased autonomy during adolescence leads to greater impulsivity and risk exposure.
Moreover, tracking individual changes in emotional regulation over time may reveal whether improvements or declines in regulation predict diverging risk profiles between children diagnosed with ADHD and TD children. Longitudinal analyses could also help determine whether emotional regulation
served as a protective factor or a vulnerability marker for future maladaptive risk-taking. Such findings would have meaningful implications for early intervention strategies, particularly if emotional regulation proves to be a modifiable factor in reducing risk behavior in youth diagnosed with ADHD.
Appendix
A) 
B) 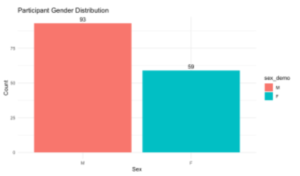
C) 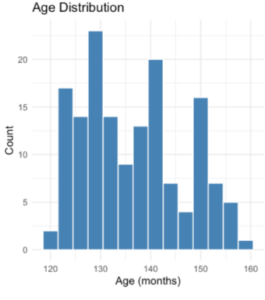
D) 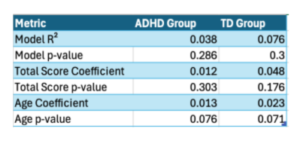
Bibliography
Asadi , H., Shoham, R., & Pollak, Y. (2021). Intertwined associations among attachment styles, emotional dysregulation, and ADHD: examining unique associations with general risk-taking behavior. Journal of Neural Transmission, 957-968.
Bunford, N., Evans, S. W., & Wymbs, F. (2015). ADHD and Emotion Dysregulation Among Children and Adolescents. Clin Child Fam Psychol Rev, 185–217.
Dekkers, T. J., Popma, A., Agelink van Rentergem, J. A., Bexkens, A., & Huizenga, H. M. (2016). Risky decision making in Attention-Deficit/Hyperactivity Disorder: A meta regression analysis. Clinical Psychology Review, 1-16.
Molina, B. S., Howard , A. L., Swanson, J. M., Stehli, A., Mitchell, J. T., Kennedy, T. M., . . . Hoza, B. (2018). Substance use through adolescence into early adulthood after childhood diagnosed ADHD: findings from the MTA longitudinal study. Journal of Child Psychology and Psychiatry, pp 692–702 .
Pollak, Y., Dekkers, T. J., Shoham, R., & Huizenga, H. M. (2019). Risk-Taking Behavior in Attention Deficit/Hyperactivity Disorder (ADHD): a Review of Potential Underlying Mechanisms and of Interventions. Current Psychiatry Reports, 21: 33.
Pollak, Y., Oz, A., Neventsal, O., Rabi, O., Kitrossky, L., & Maeir, A. (2016). Do Adolescents With Attention-Deficit/Hyperactivity Disorder Show Risk Seeking? Disentangling Probabilistic Decision Making by Equalizing the Favorability of Alternatives. Journal of Abnormal Psychology , 387–398 .
Shoham, R., Sonuga-Barke, E. J., Aloni, H., Yaniv, I., & Pollak, Y. (2016). ADHD-associated risk taking is linked to exaggerated views of the benefits of positive outcomes. Scientific Reports , 1-8.
Stralen, J. v. (2016). Emotional dysregulation in children with attention-deficit/ hyperactivity disorder. ADHD Atten Def Hyp Disord, 175–187.
