Food Allergy and Socioeconomic Status: Minimizing the Effects of Socioeconomic Status on Access to Food Allergy Treatments

Food allergies have become increasingly prevalent in the United States. The most common type of food allergy is Immunoglobulin E (IgE) mediated food allergy, in which IgE-antibodies present in the blood signal that proteins from a certain food do not belong there, which then triggers an immune response. This type of food allergy tends to develop during childhood and allergic reactions result in anaphylactic shock, an overproduction of histamine in the body in response to the detection of an allergen. This causes narrowing of airways, making it hard for a person to breathe, in addition to causing other symptoms such as low blood pressure and skin reactions like hives. Epinephrine can reduce the effects of anaphylaxis, the leading cause of food allergy related death, long enough for a person to obtain medical care. Despite epinephrine being a life-saving medication, an alarming amount of people in the United States with food allergies do not have epinephrine auto-injectors due to their expensive annual cost. Without health insurance, epinephrine can cost upwards of $500, making the medication inaccessible to a large part of the population. Additionally, health insurance does not often cover experimental new food allergy treatments (immunotherapies and biologics) which could help significantly reduce a person’s adverse reactions to allergens. This limits access to beneficial treatments to those of a higher socioeconomic status, who can afford to pay out of pocket. While some steps have been taken to make epinephrine more accessible, slightly decreasing socioeconomic effects on access to food allergies, further steps need to be taken to ensure that anyone who needs an epinephrine auto-injector is able to obtain one regardless of socioeconomic status. Until either a price-cap is placed on the cost of epinephrine auto-injectors and other food allergy treatments, or the government actively works to regulate these prices, there will continue to be inequitable access to healthcare in the United States.
Auvi-Q, EpiPen, and SYMJEPI are the three central manufacturers of epinephrine devices in the United States, with some authorized generic versions available for purchase as well (Epinephrine Options). The prices for these auto-injectors are continuously rising: the average retail price of an EpiPen on GoodRx is $689.29, not accounting for price fluctuations between pharmacies and states. Similarly, the average retail price of an auto-injector from Auvi-Q is $866.81 and $300 from SYMJEPI. For every company, this is more than double the increase in price. In 2007, an EpiPen retailed for $57, marking 400% increase in price over 15 years (Willingham). The rate at which these prices are increasing is not sustainable, making necessary medication for those with IgE-mediated food allergies unattainable.
When someone in the United States thinks of an epinephrine auto-injector, they immediately associate it with the brand EpiPen. This reflects a near monopoly governing the production and distribution of epinephrine auto-injectors. Because of this power in the market and the elasticity of demand for epinephrine as a necessary good, the three main companies that sell epinephrine auto-injectors can continue to increase their prices with little push back. Despite generic versions of epinephrine auto-injectors being available for purchase, they are not very well known, and most parents are wary of giving their children generic medications for fear that they do not work as well. Conversely, when adults experience food allergies, most choose to forgo purchasing an epinephrine auto-injector. Only 24% of adults surveyed with food allergies in the United States reported having current epinephrine prescriptions (Gupta). This leaves 76% of adults with food allergies at risk of fatal anaphylaxis, since not immediately administering epinephrine after an allergic reaction significantly increases the likelihood of death. Regardless of socioeconomic status, people do not want to spend hundreds of dollars a year on a medication that is, in best case scenarios, only going to expire and require that they purchase it again.
It is also important to note that epinephrine auto-injectors require a prescription, meaning that an additional cost is incurred by a doctor’s visit. Most health insurance policies do not cover allergist visits, particularly those in which the doctor tests for food allergies. Additionally, parents tend to purchase more than one pack of epinephrine auto-injectors, since one pack needs to be given to the school and one needs to be kept with the parent. This only incurs further annual costs.
In discussion of the total societal costs of food allergy in the United States, immunologist and lead researcher Marcus Shaker highlights that “[in 2013] food allergy had a societal cost of $24.8 billion ($4,184/affected individual) and indicated that these costs burdens were not experienced equally along racial/ethnic and socioeconomic demographics” (Shaker et al.). Additionally, direct medical costs were estimated to be $4.3 billion per year (including hospitalizations, emergency department visits, and specialist visits), while out-of-pocket, lost labor productivity, and opportunity costs totaled to about $20.5 billion a year (Gupta). This furthers the notion socioeconomic status impacts the reality of food allergies. Not only do the average costs associated with food allergy vary among different demographics (due to differences in out-of- pocket payment totals among other expenses), the feasibility of affording these costs lessens significantly when referring to people in different socioeconomic states.
Professor of Pediatrics and Medicine at Northwestern University writes: “African American and Hispanic children are significantly less likely to have formal diagnosis of food allergy…[and] children from higher income households are more likely…to be prescribed epinephrine auto-injectors…[because] wealthier families may have an easier time accessing healthcare resources,” (Gupta et al.).
Because people in these demographics are not as likely to have formal food allergy diagnoses, they are not prescribed epinephrine auto-injectors regardless of their ability to afford them in the first place. Some data suggests that African American and Hispanic children have food allergies at lower rates than those of other demographics. However, fewer formal diagnoses do not necessarily correlate to a genetic predisposition to less allergies. Further research should be done in this field to determine whether race and genetics correlate to food allergies. All of this results in an inequitable health care experience, putting those in lower socioeconomic groups at two disadvantages: (1) acquiring preventative care through allergy testing, and (2) acquiring life-saving epinephrine in the event of anaphylaxis.
One solution is to make testing for food allergies more accessible and affordable. This would increase the number of people with food allergies who have current epinephrine auto- injector prescriptions, allowing them the opportunity to obtain the medication. This solution would also need to be supplemented by a cap on the price of auto-injectors to make treatment more accessible to individuals of a lower socioeconomic status. The Inflation Reduction Act reflects a step towards progress as it includes such a price cap. Additionally, ensuring that health insurance plans cover a larger portion of the price of epinephrine auto-injectors would help ensure that at least the insured population of the United States can afford their epinephrine. Considering the costs that this would incur on both the manufacturers and distributors of this treatment, as well as the government, it is important to determine whether these possible solutions are feasible.
Epinephrine is an inexpensive drug, but the automatic injection mechanism is expensive to manufacture. Additionally, some epinephrine auto-injectors, particularly Auvi-Q brand auto- injectors, use audio mechanisms to instruct people how to use them in the event of anaphylaxis. While this is an extremely helpful feature, especially for those who have never had to use an epinephrine auto-injector before, it makes the auto-injector more expensive.
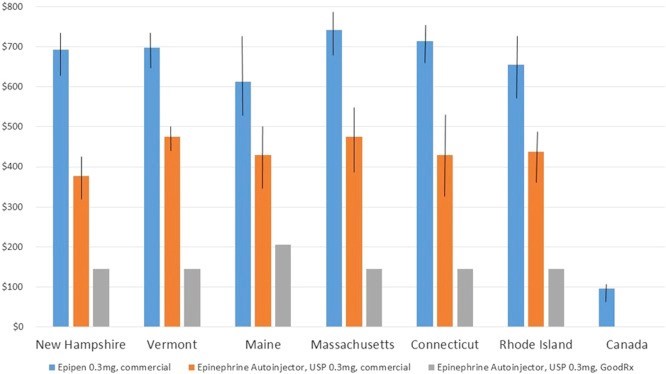
Figure 1: Pharmacy costs of epinephrine auto-injectors (Sircherer)
It is important to consider, however, that high epinephrine auto-injector prices are not unique to the United States. As seen in Figure 1, in Canada the average cost of a single epinephrine auto-injector is $96. Despite the overall epinephrine costs being less compared to the United States’ privatized healthcare system, paying $96 per epinephrine auto-injector on a yearly basis is still unsustainable for America’s poorest families. This extreme price difference reflects the need for a price cap on epinephrine, which would greatly relieve the financial burden of these prescriptions.
While the Food Allergy Research and Education (FARE) organization has put initiatives in place to make undesignated epinephrine auto-injectors more accessible in public places (as part of an initiative to reduce the effects of socioeconomic status on access to food allergy treatment), this does not completely reduce these effects. Considering that public venues like restaurants are not mandated by the government to have epinephrine auto-injectors stocked, there is no guarantee as to whether they will be available when needed. This means that people who rely on epinephrine auto-injectors are taking a significant risk if they do not have their prescribed auto-injector when going out to eat or going to school (Access to Epinephrine).
While there have been initiatives to increase access to undesignated epinephrine auto- injectors that can be stocked in places like schools and public venues, these initiatives do not fully eliminate the effects of socioeconomic status on access to effective food allergy treatment, because they do not account for anaphylaxis that happens in private residences or public places in which epinephrine is not stocked. Inability to own a prescribed epinephrine auto-injector puts individuals at significant risk of having an allergic reaction without an auto-injector on hand.
Epinephrine will continue to be a medication that many people in the United States cannot afford, resulting in an increase of anaphylaxis-related fatalities in the future unless: the manufacturing of epinephrine auto-injectors becomes more cost-efficient, companies like EpiPen are held accountable for their extremely high prices, these prices are regulated by the government, and food allergy diagnosis testing is made more accessible. In the meantime, healthcare professionals must further educate the public about food allergies and the problems associated with the high costs of epinephrine auto-injectors. Informing people about these issues can inspire them to act and find solutions, so that no child or parent needs to worry about affording an epinephrine auto-injector ever again.
References
“Access to Epinephrine.” FoodAllergy.org. https://www.foodallergy.org/resources/access- epinephrine.
“Epinephrine Options and Training.” FoodAllergy.org. https://www.foodallergy.org/resources/epinephrine-options-and-training.
Gupta, Ruchi S., Alexander M. Mitts, Madeline M. Walkner, and Alana Otto. “A Review of the Distribution and Costs of Food Allergy.” Food Allergens: Food, Microbiology, and Food Safety, pp. 19-53, 18 Nov. 2017. https://doi.org/10.1007/978-3-319-66586-3_2.
Shaker, Marcus, Joseph M. Chalil, Oth Tran, Anna Vlahiotis, Hemal Shah, Timothy King, Todd Green, and Matthew Greenhawt. “Commercial Claims Costs Related to Health Care Resource Use Associated with a Diagnosis of Peanut Allergy.” Annals of Allergy, Asthma & Immunology, vol. 124, no. 4, 2020. https://doi.org/10.1016/j.anai.2020.01.004.
Sicherer, Scott H., MD and Hugh A. Sampson MD. 2010. “Food Allergy.” Journal of Allergy and Clinical Immunology, vol. 125, no. 2, 30 Dec. 2009. https://doi.org/10.1016/j.jaci.2009.08.028
Willingham, Emily. “Why did Mylan hike EpiPen prices 400%? Because they could.” Forbes, 12 Oct. 2022. https://www.forbes.com/sites/emilywillingham/2016/08/21/why-did-mylan-hike-epipen- prices-400-because-they-could/?sh=7fc106b8280c.
